Let’s begin with the basics. Diabetes occurs whenever your pancreas doesn’t make enough insulin. This means your body is unable to regulate the levels of blood glucose, also known as blood sugar. To the unversed, blood glucose is the primary source of energy for your body. Without insulin, glucose stays in your blood, which, over time, can result in a variety of health problems. One particular part of the body that gets affected by diabetes is your skin. Yes, you heard that right: diabetes triggers a variety of skin conditions, which can be a great indicator for you to visit a diabetologist. In this post, we will learn how diabetes affects your skin by understanding the different skin conditions caused by this disease.
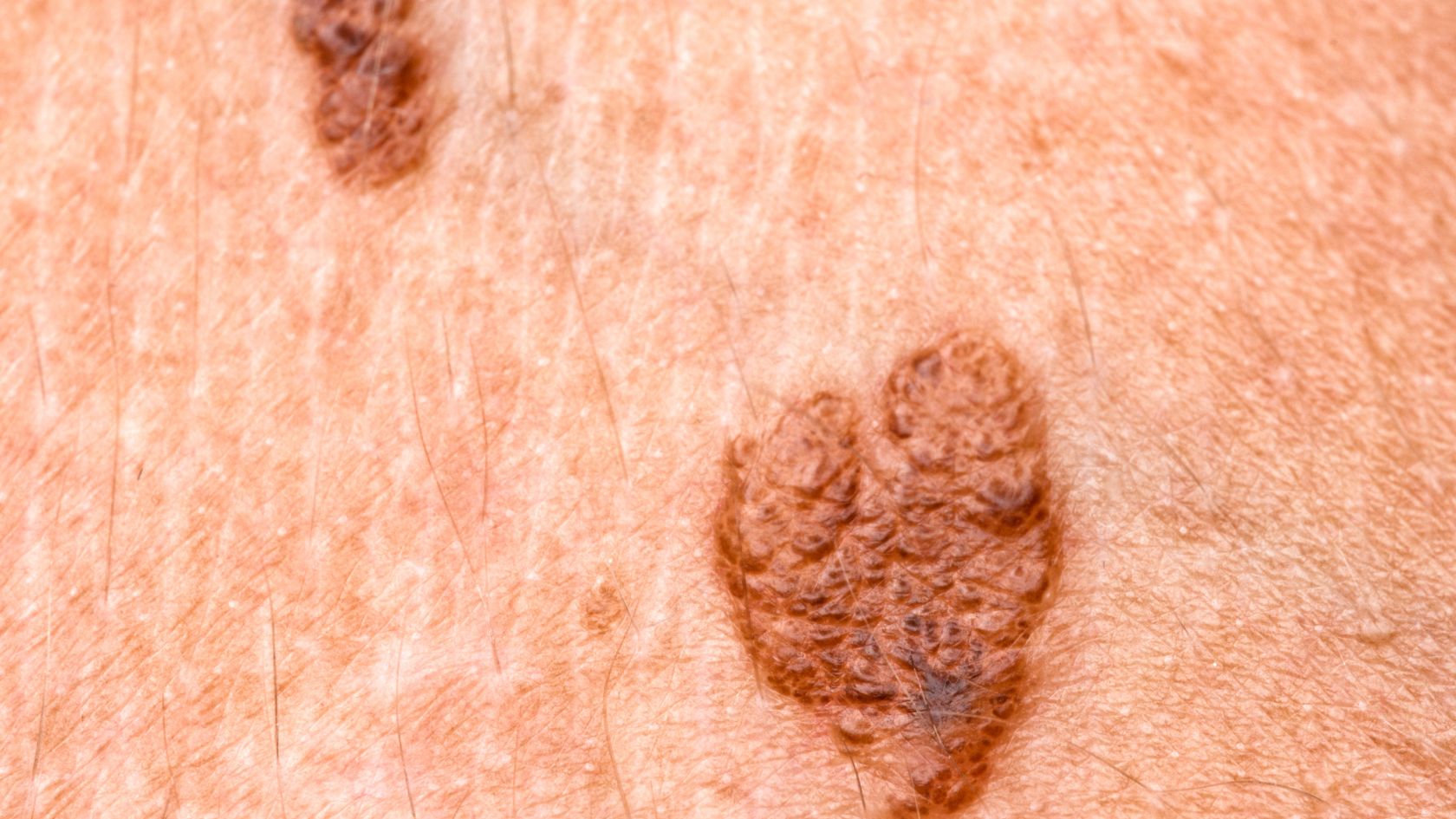
1. Acanthosis Nigricans (AN)
If you have a dark patch or strip of velvety skin, then it is Acanthosis Nigricans(AN). This usually appears in areas where creases form, such as the neck, armpits, and groin. Rarely the patches can appear on your hands, elbows, or knees. If the doctor has diagnosed it as AN, then it is due to insulin resistance, which can be indicative of prediabetes or type 2 diabetes. AN is common among those with obese bodies.
2. Diabetic Dermopathy
If you notice red or brown round patches or lines in the front of your legs (also known as shin), it could be diabetic dermopathy. It is caused due to changes in blood vessels that end up reducing the blood supply to the skin. Also known as shin spots, this condition is typically harmless in itself but can be an excellent indicator of diabetes. They neither hurt nor itch nor open up. Many people confuse it with age spots. Since the condition is harmless, you don’t have to do anything for it apart from managing your diabetes.
3. Bullosis Diabeticorum (Diabetic Blisters)
If you have burn blisters developing on your lower legs and feet, it could be Bullosis Diabeticorum, which is also known as Diabetic Blisters. While this condition looks pretty scary, they are relatively painless and heal on their own as long as you take steps to control your diabetes. This condition typically comes up only when your blood sugars are high over time. Many blisters heal on their own and seldom leave a scar. Most people find it during regular inspection of feet and skin.
4. Digital sclerosis
If you notice an onset of tight, thick, waxy skin on your fingers, then it could be digital sclerosis, which often indicates type 1 diabetes. It can also cause your finger joints to become stiff and hard to move. When the blood sugar levels remain high for a longer time, this condition can worsen, making your skin hard, thick, and swollen. The worst part – it can spread throughout your body. Unfortunately, the only way to treat digital sclerosis is by bringing blood sugar levels to normal range.
5. Bacterial infections
While bacterial infections are common even if you don’t have diabetes, the chances of getting them are higher if you have high glucose levels. The logic is pretty simple – Bacteria thrive well when there is too much sugar in your body. One of the most common bacterial infections affecting those with diabetes is staphylococcus (staph). Bacterial infections make your tissue inflamed and painful, particularly in areas like eyelids, hair follicles, and fingernails. Bacterial infections can be treated with antibiotics, but to avoid the condition, it is best to keep your diabetes under control.
6. Fungal infections
Like bacterial infections, anyone can get fungal infections, but the chances of getting the same are higher for those with diabetes. While it is not necessary, but if you regularly find itchy rashes surrounded by blisters and scales in warm and moist folds of your skin, it could indicate diabetes. The most common fungal infections include ringworm, vaginal infections, jock itch, and athlete’s foot.
7. Scleredema diabeticorum
Sometimes, you might get hard, thick, and swollen-looking skin. This is possible even when you control diabetes. This condition is called scleredema diabeticorum. It often develops on the upper back, where the skin thickens and tightens. It might happen over months or even years. Sometimes, you can also find this condition on the shoulders and neck, but never on the hands and feet. Even though the condition is painless, people might experience discoloration at the affected area.
8. Dry itchy skin
Poor circulation is more likely when you have diabetes. This is usually one of the main reasons why people with diabetes have dry, itchy skin. When you have too much sugar in the blood, it can cause the body to pull fluid from the cells. This is done to produce sufficient urine to remove excess sugar. When this happens, your skin can become dry. Apart from controlling your diabetes, you can limit your time in hot showers, use mild soaps, and use moisturizer after showering. Exercise is another way to improve circulation.
Wrap Up
We know it can take a lot of work to get your diabetes under control. However, the results are worth it. Some of the skin conditions mentioned above are not treatable unless you bring down your blood glucose levels. Knowing how diabetes affects your skin is the first step. Second, you must start getting your diabetes under control. Finally, visit a dermatologist who will help speed up the healing process of the affected skin. If you are in Bangalore or its vicinity, consult Dr. Renu Nair to effectively manage the above skin conditions. Book an appointment today.